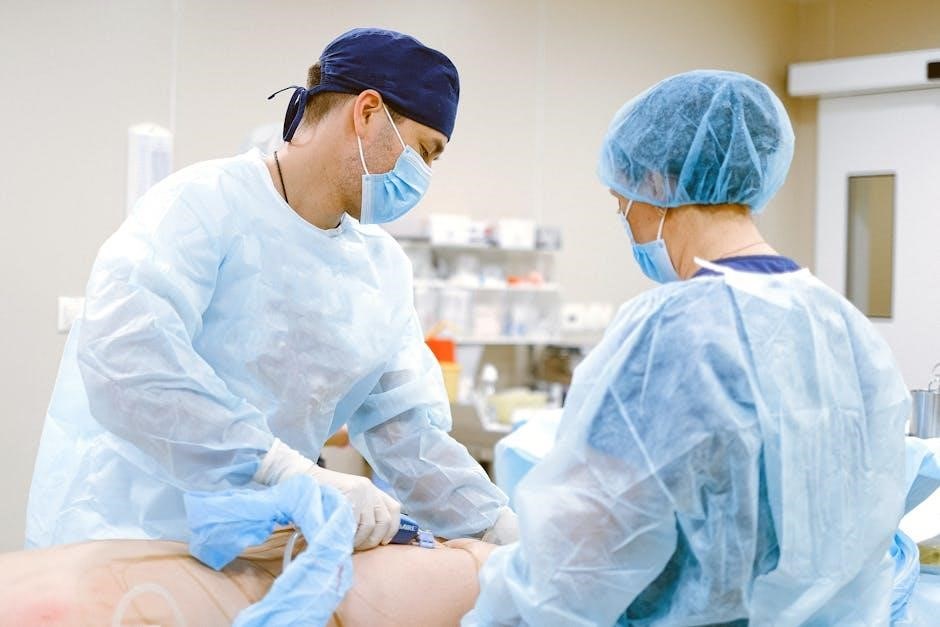
The operating room (OR) is a complex environment demanding meticulous attention to detail, where surgical procedures are performed to diagnose or treat illnesses.
Approximately 2-5% of surgical patients experience surgical site infections (SSIs), highlighting the critical need for stringent protocols and safety measures.
A standardized surgical safety checklist, inspired by aviation practices, has demonstrably reduced complications and improved patient outcomes within the OR setting.
This pocket guide emphasizes the importance of checklists, site marking, and fire risk assessments for optimal patient safety during surgical interventions.
What is an Operating Room?
The operating room (OR) represents a highly specialized hospital environment designed and equipped for performing surgical procedures. It’s a carefully controlled space, prioritizing patient safety and minimizing the risk of infection. Beyond simply a room, the OR is a system – a confluence of advanced technology, rigorously trained personnel, and standardized protocols.
This dedicated space must maintain strict aseptic conditions, employing advanced ventilation systems and sterilization techniques to prevent surgical site infections (SSIs), which affect 2-5% of surgical patients. The OR isn’t just about the surgery itself; it encompasses the entire perioperative process, from patient preparation to immediate post-operative care.
A crucial element is the implementation of safety checklists, modeled after aviation protocols, to minimize errors and enhance communication among the surgical team. These checklists, alongside procedures like marking the surgical site, are vital components of a safe and effective OR environment. The OR is a dynamic, high-stakes area demanding constant vigilance and adherence to best practices.
The Operating Room Team
A successful surgical outcome hinges on the coordinated efforts of a multidisciplinary team within the operating room. This team extends far beyond the surgeon, encompassing a diverse range of skilled professionals dedicated to patient safety and well-being.
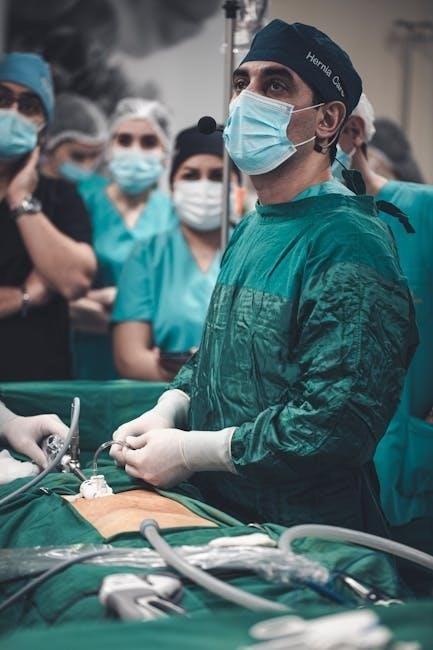
Key members include anesthesiologists, responsible for patient monitoring and pain management; surgical nurses, providing direct patient care and assisting the surgeon; and surgical technicians, preparing the OR and instruments. Additional personnel, such as perfusionists and radiology technicians, may be involved depending on the procedure.
Effective communication and collaboration are paramount, reinforced by the use of standardized checklists. These checklists ensure all team members confirm critical steps before, during, and after surgery, minimizing errors and promoting a culture of safety. The team’s collective expertise and adherence to protocols are essential in mitigating risks, including potential complications like airway failure or hemorrhage.
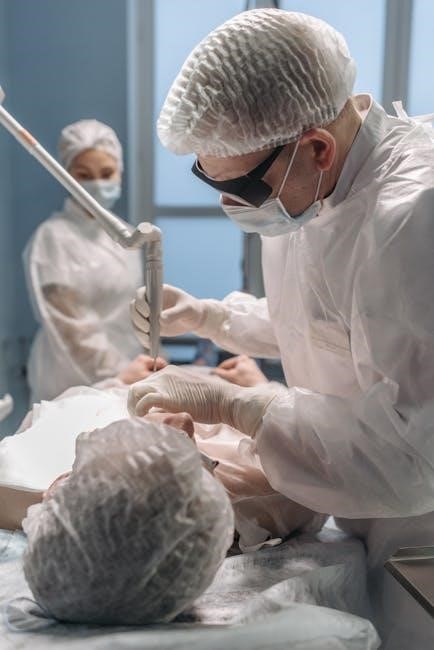
Patient Preparation
Thorough patient preparation is crucial, encompassing pre-operative assessments, obtaining informed consent, and carefully considering anesthesia needs for a safe procedure.
Prioritize patient well-being through meticulous planning and communication.
Pre-operative Assessment
A comprehensive pre-operative assessment is the cornerstone of patient safety, initiating well before the day of surgery. This involves a detailed review of the patient’s medical history, including pre-existing conditions, allergies, current medications, and previous surgical experiences.
Physical examinations are essential, focusing on cardiovascular, respiratory, and neurological function to identify potential risks. Laboratory tests, such as blood counts, coagulation studies, and electrolyte levels, provide crucial baseline data.
Furthermore, assessing the patient’s psychological state and addressing any anxieties is paramount. A thorough assessment allows the surgical team to anticipate and mitigate potential complications, tailoring the anesthetic plan and surgical approach to the individual patient’s needs.
Effective communication with the patient and their family regarding the surgical procedure, potential risks, and expected outcomes is also a vital component of this stage.
Informed Consent
Obtaining truly informed consent is a fundamental ethical and legal requirement before any surgical procedure. This process extends beyond simply having the patient sign a form; it necessitates a clear, comprehensive discussion between the surgeon and the patient.
The surgeon must explain the nature of the surgery, its potential benefits, and the inherent risks involved, including the possibility of complications. Alternative treatment options, along with their respective risks and benefits, should also be discussed.
The patient must demonstrate an understanding of this information and have the opportunity to ask questions. Documentation of this discussion, alongside the signed consent form, is crucial.
Informed consent ensures the patient’s autonomy and allows them to actively participate in decisions regarding their own healthcare, fostering trust and a collaborative relationship with the surgical team.
Anesthesia Considerations
Anesthesia plays a vital role in ensuring patient comfort and safety during surgical procedures. Careful consideration must be given to the patient’s medical history, allergies, and current medications to select the most appropriate anesthetic technique.
Common types include general anesthesia, regional anesthesia (spinal, epidural), and local anesthesia. Each has its own advantages and disadvantages, and the choice depends on the surgery’s complexity, patient health, and surgeon preference.
Potential complications, such as failed airway management, hypoxia, and bronchospasm, require vigilant monitoring and prompt intervention.
The anesthesia team continuously monitors vital signs – heart rate, blood pressure, oxygen saturation, and respiratory rate – throughout the procedure, adjusting medication as needed to maintain patient stability.
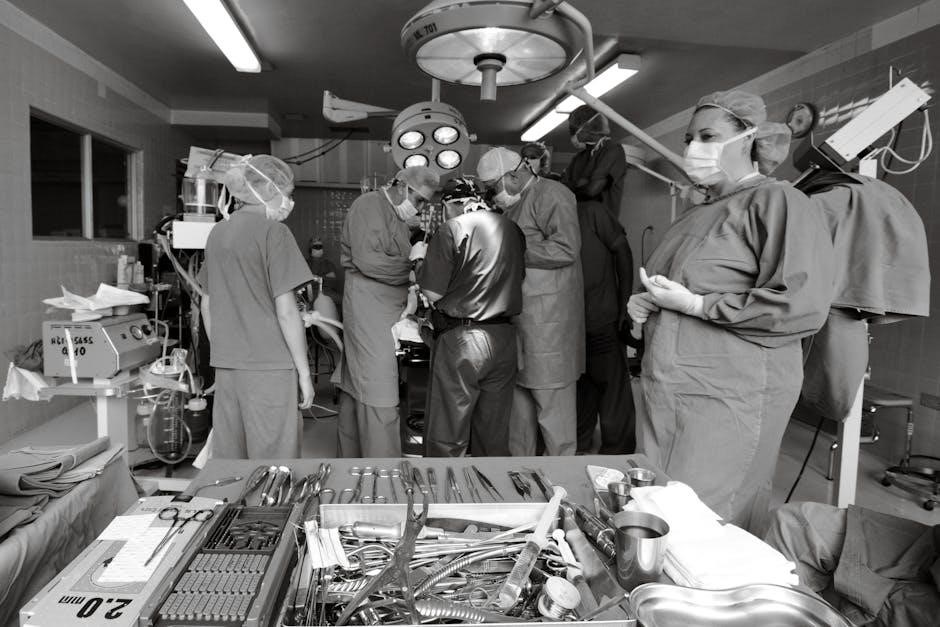
Surgical Safety
Prioritizing surgical safety is paramount, utilizing checklists before, during, and after procedures to minimize risks and enhance patient well-being within the OR.
Effective site marking and thorough fire risk assessments are crucial components of a safe surgical environment, preventing errors and complications.
Surgical Safety Checklist
The Surgical Safety Checklist, modeled after aviation protocols, is a vital tool for enhancing patient safety and reducing complications in the operating room. This checklist is typically implemented in three phases: before anesthesia, before skin incision, and before the patient leaves the operating room.
Before anesthesia, verification of patient identity, surgical site, and allergies is essential. Confirmation of anesthesia equipment and availability of necessary supplies are also critical steps. Prior to skin incision, the surgical team confirms the correct procedure, surgical site marking, and addresses any potential concerns.
Finally, before the patient leaves the OR, the team verifies the completion of instrument, sponge, and needle counts, reviews any specimen labeling, and confirms any immediate post-operative concerns. Consistent and diligent use of this checklist significantly minimizes preventable errors and promotes a culture of safety.
Adherence to this standardized process is key to improved outcomes.
Marking the Surgical Site
Accurate surgical site marking is a cornerstone of patient safety, preventing errors and ensuring the correct procedure is performed on the intended location. This practice involves the surgeon clearly marking the surgical site before the patient enters the operating room, ideally with the patient involved in the process.
The marking should be done in a location visible after the patient is positioned and prepped for surgery. It must be unambiguous and correspond to the planned incision site. Accepted methods include initialing the site or using a permanent marker.
Site marking is particularly crucial for procedures involving bilateral structures or multiple potential sites. It’s a non-negotiable step, and documentation of the marking process is essential. Failure to properly mark the site can lead to devastating consequences, emphasizing its importance in the surgical workflow.
Standardization is key to effective implementation.
Operating Room Fire Risk Assessment
The operating room presents a unique fire hazard due to the combination of high concentrations of oxygen, flammable substances like alcohol-based skin preps, and ignition sources such as electrosurgical devices. A thorough fire risk assessment is therefore paramount before initiating any surgical procedure.
This assessment involves identifying potential fuel sources – including surgical drapes, prepping solutions, and patient skin – and minimizing their presence. Oxygen levels should be carefully monitored and adjusted. Electrosurgical units must be tested for proper grounding and function.
Fire carts containing appropriate extinguishing agents (typically carbon dioxide extinguishers) must be readily accessible and staff trained in their use. Awareness of the “fire triangle” – fuel, oxygen, and ignition source – is crucial for prevention.
Regular drills and adherence to established operating room fire guidelines are essential for maintaining a safe environment.
Common Operating Room Emergencies
Rapid recognition and management of emergencies are vital; potential crises include failed airways, hypoxia, bronchospasm, pneumothorax, and significant hemorrhage requiring immediate intervention.
Preparedness and swift action are key to positive patient outcomes during unexpected critical events within the operating room environment.
Failed Airway Management
A failed airway is a critical emergency demanding immediate and decisive action within the operating room. This occurs when intubation or ventilation attempts are unsuccessful, leading to potential hypoxia and requiring alternative airway strategies.
Initial steps involve confirming endotracheal tube placement, assessing for anatomical obstructions, and utilizing adjuncts like a laryngeal mask airway (LMA). If these fail, a surgical airway – cricothyrotomy – may be necessary to establish a definitive airway.
Effective communication and a coordinated team response are paramount. Having a pre-defined “difficult airway” protocol, including readily available equipment (fiberoptic bronchoscope, bougie, cricothyrotomy kit), is crucial. Continuous monitoring of oxygen saturation and capnography guides interventions.
Remember the mnemonic “DOPE” (Displacement, Obstruction, Pneumothorax, Equipment failure) to systematically troubleshoot the cause of airway compromise. Prompt recognition and skilled management significantly improve patient safety.
Hypoxia and Oxygen Administration
Hypoxia, a deficiency in oxygen reaching tissues, is a potentially life-threatening complication in the operating room requiring rapid identification and intervention. Recognizing early signs – desaturation noted on pulse oximetry, altered mental status, and increased heart rate – is critical.
Immediate oxygen administration is the first step, typically via a non-rebreather mask delivering 100% oxygen. Simultaneously, investigate the underlying cause: inadequate ventilation, airway obstruction, or cardiovascular compromise.
Assess the patient’s respiratory effort and auscultate lung sounds. If hypoxia persists, consider assisted ventilation with a bag-valve-mask or, if necessary, re-intubation.
Continuous monitoring of oxygen saturation, end-tidal CO2, and arterial blood gases guides treatment. Promptly address the root cause while maximizing oxygen delivery to prevent further deterioration and ensure patient stability.
Hemorrhage Control
Uncontrolled hemorrhage represents a significant threat during surgical procedures, demanding swift and decisive action. Initial management focuses on direct pressure to the bleeding site, utilizing sterile gauze or surgical sponges. Elevation of the affected limb can also aid in reducing blood flow.
If direct pressure is insufficient, consider applying a tourniquet proximal to the bleeding source for extremity hemorrhage. Simultaneously, summon assistance and prepare for potential blood product transfusion.
Identifying the source of bleeding is paramount; meticulous surgical technique and thorough exploration are essential. Employ electrocautery or suture ligation to secure bleeding vessels.
Monitor vital signs closely – heart rate, blood pressure, and oxygen saturation – to assess the extent of blood loss and guide resuscitation efforts. Maintaining adequate circulating volume is crucial for patient survival.
Infection Control in the Operating Room
Maintaining a sterile environment is paramount to prevent surgical site infections (SSIs), impacting 2-5% of patients.
Aseptic technique, proper sterilization, and optimized airflow are crucial for patient safety.
Surgical Site Infections (SSIs)
Surgical Site Infections (SSIs) represent a significant challenge in healthcare, affecting an estimated 2 to 5 percent of patients undergoing surgical procedures. These infections not only prolong hospital stays and increase healthcare costs but also contribute to patient morbidity and, in some cases, mortality.
Effective infection control strategies within the operating room are therefore absolutely critical. Prevention hinges on a multi-faceted approach, encompassing meticulous surgical technique, rigorous adherence to aseptic protocols, appropriate preoperative skin preparation, and judicious use of prophylactic antibiotics when indicated.
Postoperative wound care, including diligent monitoring for signs of infection – redness, swelling, pain, and purulent drainage – is equally important. Early detection and prompt treatment of SSIs are essential to minimize complications and optimize patient outcomes. A comprehensive understanding of SSI risk factors and implementation of evidence-based prevention bundles are key components of a robust infection control program.
Sterilization and Aseptic Technique
Maintaining a sterile field is paramount within the operating room to prevent surgical site infections. Sterilization, the complete elimination of all microorganisms, is achieved through methods like autoclaving, utilizing high pressure and steam, or employing chemical sterilants for heat-sensitive instruments.
Aseptic technique, encompassing practices that minimize contamination, is equally vital. This includes meticulous hand hygiene by all surgical team members, proper draping of the patient to create a sterile barrier, and the use of sterile gowns, gloves, and masks.
Strict adherence to established protocols for instrument handling, cleaning, and sterilization is non-negotiable. Regular monitoring of sterilization processes, including biological indicators, ensures their effectiveness. Any breach in sterile technique must be immediately addressed to maintain patient safety and minimize the risk of postoperative complications.
Airflow and Ventilation
Operating room airflow systems are meticulously engineered to minimize the risk of airborne contamination. Positive pressure ventilation ensures that air flows from the operating room towards surrounding areas, preventing the entry of microorganisms. High-efficiency particulate air (HEPA) filters remove bacteria, viruses, and other particles, maintaining air purity.
Air exchange rates, typically 15-20 air changes per hour, dilute and remove potential contaminants. Laminar airflow systems, directing air in a unidirectional stream, create a sterile zone over the surgical site, further reducing infection risk.
Regular monitoring and maintenance of the ventilation system are crucial to ensure optimal performance. Proper functioning is essential for maintaining a safe and sterile environment, protecting both patients and surgical staff from airborne pathogens and contributing to reduced surgical site infection rates.
Specialized Equipment
Essential tools like the Lucas 3 and Prevalon MATS/HoverJack are vital for efficient patient handling and resuscitation during surgical procedures, ensuring optimal care.
Quick reference guides for these devices are crucial for rapid deployment in emergency situations.
Lucas 3 Quick Reference
The LUCAS 3 device provides mechanical chest compressions, offering consistent and uninterrupted CPR during cardiac arrest situations within the operating room environment. This automated system frees up personnel for other critical tasks.
Key steps for operation include ensuring the device is fully charged, correctly positioning the compression head on the sternum, and selecting the appropriate compression rate and depth based on established protocols.
Regularly verify the device’s functionality through self-tests and visual inspections. Monitor the patient’s rhythm and vital signs throughout the compression process. The LUCAS 3 is designed for ease of use, but proper training is essential for optimal performance.
Remember to document the duration of compressions and any observed changes in the patient’s condition. Always follow hospital-specific guidelines and manufacturer’s recommendations for LUCAS 3 operation and maintenance.
Proper use can significantly improve resuscitation outcomes.
Prevalon MATS / HoverJack System
The Prevalon MATS (Multi-Action Technology Surface) and HoverJack systems are designed to minimize pressure injuries during lengthy surgical procedures. These systems create a dynamic support surface, reducing interface pressure and shear forces.
The MATS utilizes a network of interconnected cells that automatically adjust to the patient’s body contours, distributing weight evenly. The HoverJack introduces a low-friction layer, allowing for easier repositioning and reducing skin damage.
Proper application involves ensuring the surface is clean and dry, correctly positioning the patient, and regularly inspecting the skin for signs of pressure or irritation. Adjust settings based on patient weight and surgical position.
Regularly assess the patient’s skin and document any changes. Familiarize yourself with the system’s controls and troubleshooting procedures. These systems are vital for maintaining skin integrity during prolonged operations.
Following instructions is key to optimal patient care.
Post-Operative Considerations
Immediate post-operative care focuses on monitoring vital signs, managing pain effectively, and preventing complications like infection.
Pain management protocols should be individualized, utilizing a multimodal approach to optimize patient comfort and recovery.
Immediate Post-Operative Care
The initial recovery period, immediately following surgery, is paramount for patient well-being and preventing adverse events. Continuous monitoring of vital signs – including heart rate, blood pressure, respiratory rate, and oxygen saturation – is essential to detect any early signs of instability.
Assess the surgical site for excessive bleeding or hematoma formation, and ensure proper wound dressing integrity; Pain assessment should be frequent and proactive, utilizing validated pain scales to guide analgesic administration.
Maintaining adequate airway patency and respiratory function is critical; encourage deep breathing exercises and monitor for signs of respiratory depression. Early mobilization, as appropriate, helps prevent complications like pneumonia and deep vein thrombosis.
Fluid balance must be carefully managed, monitoring intake and output to prevent dehydration or fluid overload. Vigilance for signs of infection, such as fever or wound inflammation, is crucial for prompt intervention.
Pain Management
Effective pain control is a cornerstone of post-operative care, significantly impacting patient recovery and satisfaction. A multimodal approach, combining different analgesic modalities, is often most effective, minimizing reliance on opioids alone.
Non-pharmacological methods, such as positioning, relaxation techniques, and distraction, can complement medication. Regularly assess pain levels using a standardized scale, documenting the intensity, character, and location of discomfort.
Opioid analgesics, when necessary, should be administered cautiously, considering potential side effects like nausea, constipation, and respiratory depression. Non-opioid options, including NSAIDs and local anesthetics, can provide effective pain relief with fewer adverse effects.
Patient education regarding pain management strategies and potential side effects is crucial. Proactive pain control, rather than reacting to escalating pain, optimizes patient comfort and facilitates early mobilization and rehabilitation.